Colorectal cancer is the 3rd most common type of cancer and the 3rd leading cause of cancer death in the United States. Colonoscopies have long been the standard screening procedure for detecting growths in the colon, but CT Colonography is a comparably accurate, non-invasive alternative. Ask your care provider to refer you to UVA Radiology and Medical Imaging for your CT Colonography.
Understanding Colorectal Cancer
Doctors usually refer to cancer in the colon or rectum as colorectal cancer. Before we talk about what colorectal cancer is and how doctors screen for it, it’s helpful to know where the colon and rectum are and what they do.
The colon (also known as the large intestine) and rectum are the final parts of the body’s digestive system. After food is swallowed it enters the stomach, where digestive juices begin to break it down. A thick slurry of solid food and liquid passes from the stomach to the small intestine, where nutrients are absorbed into the bloodstream. Next, the material moves to the colon, where the liquid is absorbed and the remaining solid material is passed to the rectum. The rectum connects the colon to the anus. It’s where this solid material, or stool, is stored until it is eliminated from the body.
Abnormal collections of cells called polyps can attach to and grow on the inner lining of the colon or rectum. Most polyps are non-cancerous, but colorectal cancer often develops from one particular type of polyp, called adenomas. The goal of a colorectal cancer screening is to detect and remove adenomas and other polyps as early as possible, before they become cancerous.
Who Should Be Screened?
According to the American Cancer Society, everyone aged 45 to 75 should be screened for colorectal cancer. People at a greater risk include anyone over 60 years old, and anyone with a family or personal history of colorectal cancer, inflammatory bowel disease, or cancer of the ovary, breast or endometrium. Smoking cigarettes, drinking alcohol regularly or consuming a high-fat, low-fiber diet also put you at increased risk for colorectal cancer.
Traditional Colonoscopy vs. CT Colonography
A traditional colonoscopy is the most widely known colorectal cancer screening procedure, but many patients are choosing a non-invasive CT (computerized tomography) Colonography instead. A CT Colonography doesn’t require sedation and is just as accurate at detecting most precancerous polyps.
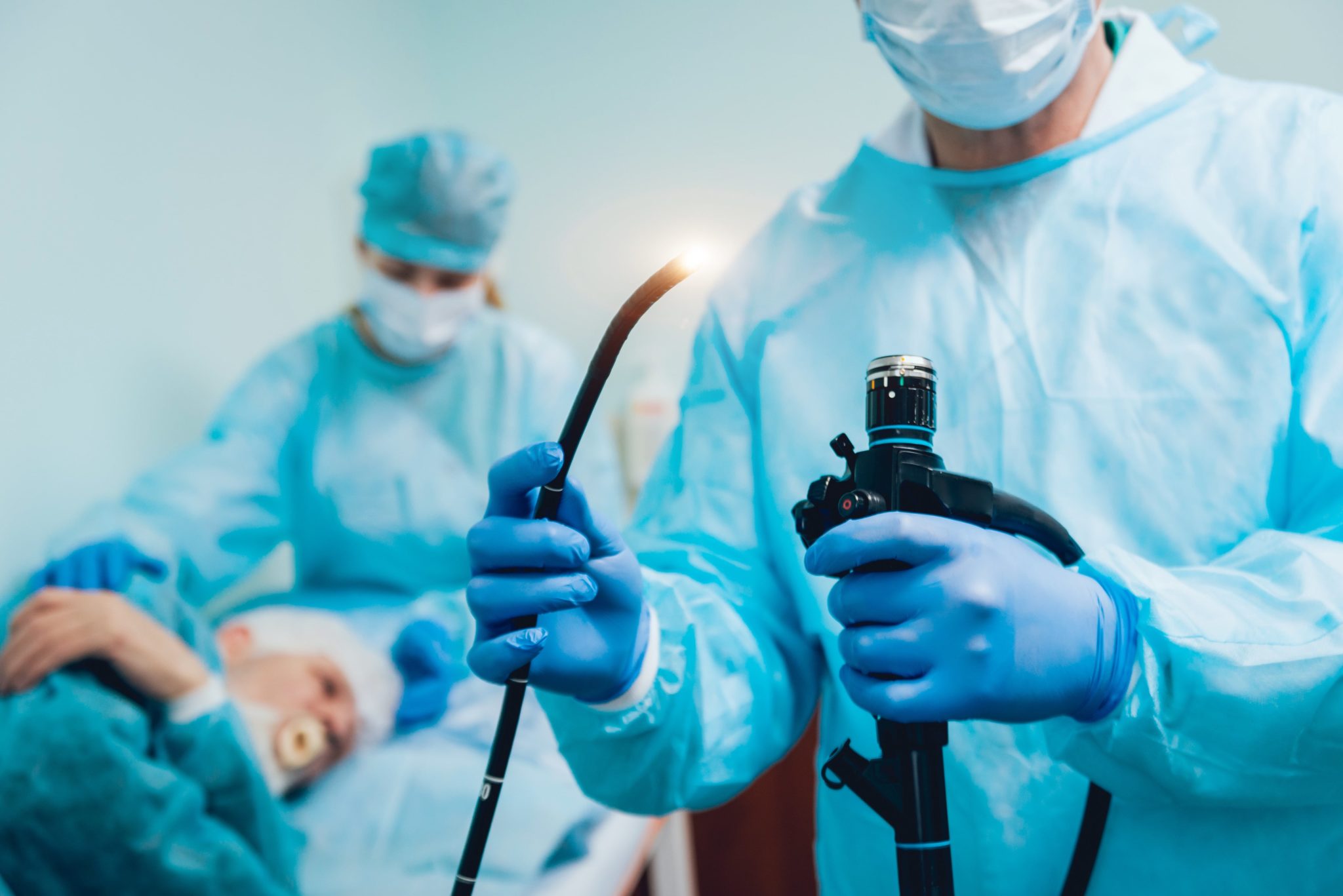
For a traditional colonoscopy, a doctor inserts a flexible metal tube with a camera on the end into the colon through the rectum. The tube is maneuvered through the entire length of the colon, which is usually 5 to 6 feet long. If a doctor finds a polyp during a colonoscopy, he or she can remove it without the need for another procedure. Because the tube is inserted throughout the entire colon, there is a slight risk of colon perforation or bleeding.
During a CT Colonography, a small tube is inserted a few inches into the rectum to gently inflate the colon with gas or air. This helps make the images of the colon clearer. A low-dose radiation CT Scanner then produces images of the entire colon. If polyps are found, however, an additional colonoscopy will be needed to remove them.
Both screening procedures require bowel cleansing to ensure that the colon and rectum are empty.
We’ve created this diagram to show you a few other key differences between a traditional colonoscopy and a CT Colonography:
To schedule a non-invasive CT Colonography, speak with your care provider. To learn more about imaging specialties or procedures performed by the highly skilled radiologists at UVA, visit https://uvahealth.com/services/imaging or call (434) 243-0321.
Infographic Text: Traditional Colonoscopy vs. CT Colonography
-
Traditional Colonoscopy
-
45-60 minutes
-
5-6 feet of tubing
-
Usually requires sedation
-
No radiation
-
Entire colon screened
-
-
CT Colonography
-
15 minutes
-
2-3 inch probe
-
No sedation
-
Low dose of radiation
-
Entire colon screened. Can also detect other issues in your abdomen.
-