Lab testing for COVID-19 (also known as the novel coronavirus or SARS-CoV2) has increased greatly since the virus spread across the globe in spring 2020. Current evidence suggests that chest CT scans and x-rays are generally NOT specific enough to either diagnose or rule out COVID-19 on their own. But imaging does have a limited role to play: when used with lab tests, a medical history and a physical exam, CT scans or x-rays can be helpful for diagnosing COVID-19 or determining the severity of the disease in some patients.
What is COVID-19 and How Does it Spread?
Coronaviruses are a large family of viruses that can infect humans or animals. Usually the symptoms associated with an infection are very mild, similar to the common cold. But COVID-19 is a virus that has not been seen in humans before, which means that anyone can be infected and that no one has built-in immunity to it.
The primary symptoms of a COVID-19 infection are fever, dry cough, and shortness of breath. Some patients with COVID-19 have also reported fatigue, muscle aches, a loss of smell (anosmia) or taste, and up to 10% have GI-related symptoms such as diarrhea.
Though most cases of COVID-19 are mild, it has produced more serious symptoms in certain populations. People at a higher risk include those older than 65, those who are markedly overweight, and the immunocompromised. People who have preexisting conditions such as diabetes, heart disease, underlying lung disease, and women who are pregnant are also at risk. Click here for the Centers for Disease Control (CDC)’s information on people who may be at higher risk.

COVID-19 is more contagious and lethal than the seasonal flu. It spreads mainly by person-to-person contact. Droplets containing the viruses are expelled when an infected person talks, coughs or sneezes. These droplets can land in the mouth or noses of other people and be inhaled into their lungs. Evidence suggests that the longer and closer an infected person interacts with an uninfected person, the greater the chance of transmission.
COVID-19 can live in the air for several hours or on surfaces for 14 days or more. To avoid infection, follow these steps:
- Stand at least 6 feet away from other people. This is called social distancing.
- Wear a mask that covers your nose and mouth when around others.
- Thoroughly wash your hands often for at least 20 seconds. If you can’t wash your hands, use hand sanitizer that contains at least 60% alcohol.
- Don’t touch your face unless you have cleaned your hands well.
Click here to learn more about how to prepare for COVID-19, or to learn more about symptoms.
Diagnosing COVID-19
Identifying and isolating patients infected with COVID-19 is an important step in managing this global pandemic. To stop the spread, health care providers need to identify who infected people have come in contact with. This process is known as contact tracing.
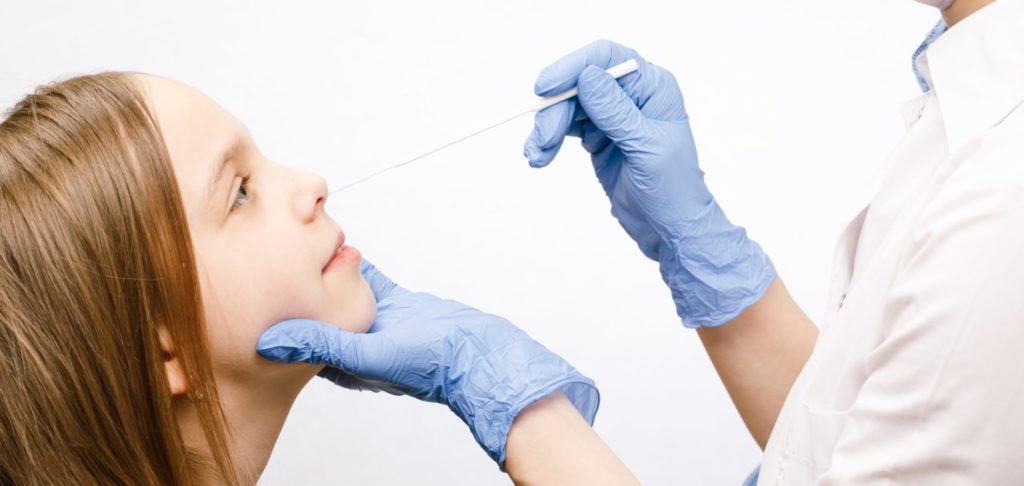
In patients who develop COVID-19-like symptoms or who meet certain travel or exposure criteria, testing is done using a special swab in the nose or back of the throat. A laboratory then checks the sample on the swab for the virus’s genetic material. Depending on the specific test, it may take from one to several days to find out the results of the test. Some centers, such as the University of Virginia, have developed a test that is performed on site with results available within 24 hours.
Before many parts of the world had adequate access to testing, some care providers tried to use imaging tests to diagnose COVID-19. This was usually done with a CT scan or chest x-ray. While patients with COVID-19 can show an abnormality on either a chest x-ray or CT scan, many other lung problems can look very similar. Additionally, the absence of an abnormality on either a chest x-ray or CT scan does not necessarily exclude COVID-19. For this reason, most experts and medical societies advise against the use of an imaging test alone to diagnose or rule out COVID-19.
The Limited Role of Chest CTs and X-Rays in Diagnosing COVID-19
The American College of Radiology (or ACR), which represents nearly 40,000 radiologists in the United States, has issued guidance that CTs and x-rays should not be used as a first-line tool to diagnose or screen for COVID-19. There are three major reasons for the ACR’s recommendation:
- A chest CT or x-ray cannot accurately distinguish between COVID-19 and other respiratory infections, like seasonal flu. Unlike swab tests, which lead to specific diagnoses of COVID-19, imaging findings are not specific enough to confirm COVID-19. They can only point to signs of an infection. Those signs could be due to other causes, including seasonal flu which is very common at certain times of year.
- A significant percentage of patients with COVID-19 have normal chest CTs or x-rays. For those patients, a normal imaging result could falsely convince them that they are healthy. If they believe they are healthy, they are at greater risk of spreading the virus to others.
- Because COVID-19 is highly contagious, using imaging equipment on COVID-19 patients is a serious hazard for healthcare providers and other patients. CT scanners are large and complex pieces of machinery. They need to be thoroughly cleaned between each potential COVID-19 patient. But even with careful cleaning, there is a risk that the virus could remain on a surface in a CT scanner room. Additionally, moving potential COVID-19 patients to and from a CT scanner room increases the risk of spreading the virus inside of healthcare facilities. It also means that fewer CT scanners would be available for other vulnerable patients who need this imaging test.
Though CT scans and x-rays aren’t recommended as the only way to diagnose COVID-19, they may be appropriate on a case-by-case basis. For patients with severe symptoms, imaging might help to assess the seriousness of the disease. And when used with lab tests, a thorough medical history and a physical exam, CT scans or x-rays can be helpful for determining a plan of care for a patient.
Taking Appropriate Steps for Your Health
Overall, imaging plays a complementary role in the management of patients with COVID-19. It is not recommended as a sole screening tool. Currently, laboratory tests are the most accurate method of diagnosing this disease. They are also the only method the CDC currently endorses.
If you or a loved one are concerned that you might have coronavirus, speak to your healthcare provider by phone before coming to a healthcare facility. Contact your provider immediately if you have any of the CDC’s emergency warning signs for COVID-19, including trouble breathing or persistent chest pain. If you have symptoms but don’t have access to a laboratory test, stay home and follow the CDC’s guidelines for protecting others.
To learn more about what UVA Health is doing to protect our patients from COVID-19, as well as protocols for seeking treatment or testing, please visit UVA Health’s Coronavirus page. For more information about COVID-19, visit the CDC’s Coronavirus webpage.
Article reviewed and edited by Arun Krishnaraj, MD, MPH, and Alan Matsumoto, MD. Last updated 9/21/2021.